Definition 1
A urinary tract infection (UTI) is an infection that affects part of the urinary tract.[1]

Definition 2
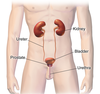
When it affects the lower urinary tract it is known as a bladder infection (cystitis) and when it affects the upper urinary tract it is known as kidney infection (pyelonephritis).[2]
Symptoms 1
Symptoms from a lower urinary tract include pain with urination, frequent urination, and feeling the need to urinate despite having an empty bladder.[1]

Symptoms 2
Symptoms of a kidney infection include fever and flank pain usually in addition to the symptoms of a lower UTI.[2] Rarely the urine may appear bloody.[3]

Symptoms 3
In the very old and the very young, symptoms may be vague or non-specific.[1][4]

Cause
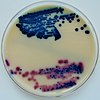
The most common cause of infection is Escherichia coli, though other bacteria or fungi may rarely be the cause.[5]

Risk factors
Risk factors include female anatomy, sexual intercourse, diabetes, obesity, and family history.[5]
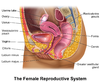
Diagnosis 1
Diagnosis in young healthy women can be based on symptoms alone.[6]

Diagnosis 2
In those with vague symptoms, diagnosis can be difficult because bacteria may be present without there being an infection.[7] In complicated cases or if treatment fails, a urine culture may be useful.[8]
Treatment 1
In uncomplicated cases, UTIs are treated with a short course of antibiotics such as nitrofurantoin or trimethoprim/sulfamethoxazole.[3] Resistance to many of the antibiotics used to treat this condition is increasing.[1]

Treatment 2
In complicated cases, a longer course or intravenous antibiotics may be needed.[3] If symptoms do not improve in two or three days, further diagnostic testing may be needed.[8]
Treatment 3
Phenazopyridine may help with symptoms.[1]

Prevention
In those with frequent infections, a short course of antibiotics may be taken as soon as symptoms begin or long-term antibiotics may be used as a preventative measure.[9]

Epidemiology 1
About 150 million people develop a urinary tract infection in a given year.[5] They are more common in women than men.[3] Up to 10% of women have a urinary tract infection in a given year, and half of women have at least one infection at some point in their lifetime.[6][3]

Epidemiology 2
They occur most frequently between the ages of 16 and 35 years.[3] Recurrences are common.[3]

History
Urinary tract infections have been described since ancient times with the first documented description in the Ebers Papyrus dated to c. 1550 BC.[10]

References
- ^ a b c d e "Urinary Tract Infection". CDC. April 17, 2015. Archived from the original on 22 February 2016. Retrieved 9 February 2016.
- ^ a b Lane, DR; Takhar, SS (August 2011). "Diagnosis and management of urinary tract infection and pyelonephritis". Emergency Medicine Clinics of North America. 29 (3): 539–52. doi:10.1016/j.emc.2011.04.001. PMID 21782073.
- ^ a b c d e f g Salvatore S, Salvatore S, Cattoni E, Siesto G, Serati M, Sorice P, Torella M (June 2011). "Urinary tract infections in women". European Journal of Obstetrics, Gynecology, and Reproductive Biology. 156 (2): 131–6. doi:10.1016/j.ejogrb.2011.01.028. PMID 21349630.
- ^ Woodford, HJ; George, J (February 2011). "Diagnosis and management of urinary infections in older people". Clinical Medicine. 11 (1): 80–3. doi:10.7861/clinmedicine.11-1-80. PMC 5873814. PMID 21404794.
- ^ a b c Flores-Mireles, AL; Walker, JN; Caparon, M; Hultgren, SJ (May 2015). "Urinary tract infections: epidemiology, mechanisms of infection and treatment options". Nature Reviews. Microbiology. 13 (5): 269–84. doi:10.1038/nrmicro3432. PMC 4457377. PMID 25853778.
- ^ a b Nicolle LE (2008). "Uncomplicated urinary tract infection in adults including uncomplicated pyelonephritis". Urol Clin North Am. 35 (1): 1–12, v. doi:10.1016/j.ucl.2007.09.004. PMID 18061019.
- ^ Jarvis, William R. (2007). Bennett & Brachman's hospital infections (5th ed.). Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins. p. 474. ISBN 9780781763837. Archived from the original on 2016-02-16.
- ^ a b Colgan R, Williams M, Johnson JR (2011-09-01). "Diagnosis and treatment of acute pyelonephritis in women". American Family Physician. 84 (5): 519–26. PMID 21888302.
- ^ "Recurrent uncomplicated cystitis in women: allowing patients to self-initiate antibiotic therapy". Rev Prescire. 23 (146): 47–9. Nov 2013. PMID 24669389.
- ^ Al-Achi, Antoine (2008). An introduction to botanical medicines : history, science, uses, and dangers. Westport, Conn.: Praeger Publishers. p. 126. ISBN 978-0-313-35009-2. Archived from the original on 2016-05-28.


Recent Comments